Boutonniere Finger Deformity
What is Boutonniere Finger?
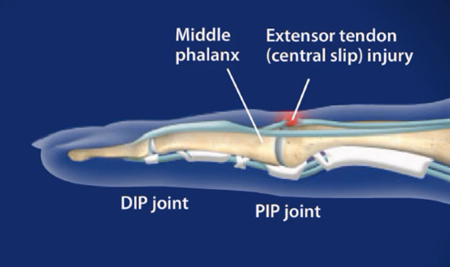
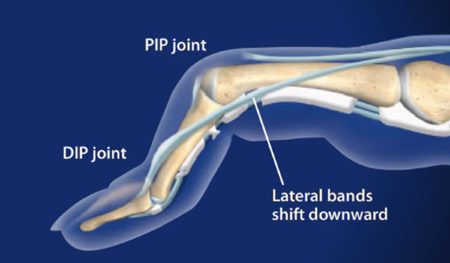
Each finger, except for the thumb, is composed of three bones with ligaments connecting bone to bone and tendons connecting muscle to bone. There are several tendons that run along the side and top of the finger that allow for movement and keep the finger straight. When the tendon that runs along the top of the middle joint of the finger (the central slip of tendon) is torn the middle joint may push its way thru the tear causing the finger to bend. The tear in the tendon resembles a “boutonniere” which is French for buttonhole. Boutonniere Finger Deformity is characterized by flexion of the middle joint (proximal interphalangeal joint) and hyperextension of the fingertip (distal interphalangeal joint).
What causes Boutonniere Finger?
Boutonniere finger may occur because of a chronic condition like rheumatoid arthritis or after acute injury. Forceful “jamming” of a finger is the most common cause. However, any injury that produces a cut to the top of the finger may have the same result.
What are the symptoms of Boutonniere Finger?
The most prominent symptom is a finger in which the bent middle joint is unable to straighten out, while the fingertip is unable to flex. Some experience pain or swelling to the finger that persists. Signs of boutonniere finger generally occur within three weeks following injury but can appear immediately dependent on mechanism of injury.
In patients with rheumatoid arthritis the deformity occurs gradually over time and is categorized into three stages. It is important to seek medical treatment early to avoid the possibility of irreversible damage.
How is Boutonniere Finger diagnosed?
Diagnosis is relatively simple due to the distinctive nature of the deformity. After a complete history is taken the doctor will examine the affected digit. The finger may be manipulated to ascertain range of motion. X-rays may be ordered to determine if there are any bone fractures.
How is Boutonniere Finger treated?
Non-surgical
Early intervention is essential to retaining full range of motion in the affected digit and non-surgical treatment is typically preferred. If not treated within the first three weeks after injury the deformity may become permanent.
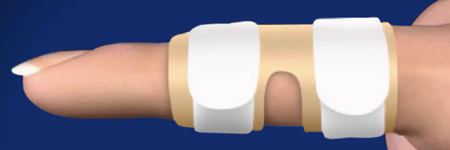
Treatment is dependent on the origin of the deformity. In traumatic injury, splinting is the most common treatment. The finger splint holds the digit in proper alignment while the tendon heals. The finger is immobilized for approximately 6 weeks. After this time some patients may be required to wear the splint at night. The doctor will likely recommend therapy and range of motion exercises during this time to restore flexibility.
Boutonniere finger caused by arthritis is managed based on the stage of the deformity. It is often treated by splinting the digit along with oral medications or injections. In some cases surgery may be indicated.
Surgical
Surgical intervention may be required for several reasons. If the condition does not improve with splinting, the tendon is severed, there is a displaced bone fragment, or in cases of severe arthritis, surgery could be the only option. Generally, the goal for surgery is to reduce pain, repair soft tissue damage and restore as much function as possible. Post operatively the finger will be splinted for 4-6 weeks. Therapy will then begin and continue for several months.
As with any surgical procedure, expectations should be discussed with the surgeon to insure congruency with typical surgical outcomes.
How can Dr. Knight help you with Boutonniere Deformity?
After confirming that you do, in fact, suffer from Boutonniere Deformity, it is important that you receive treatment as soon as possible, because if left untreated, this deformity can severely affect your manual dexterity. Once diagnosed, Dr. Knight will treat you as soon as possible in order to allay any complications that might arise, and to restore you to full mobility and dexterity, so that you can return to your life and work.
We looking forward to helping you live a more pain free life. Dr. Knight is one of the top hand doctors in Dallas. Contact us online or visit Dr. John Knight at our Southlake hand and wrist center or Dallas office location.
Boutonniere Finger Deformity Fact Sheet
| What can cause me to develop a Boutonniere deformity? | Boutonniere deformity is largely caused by underlying rheumatoid arthritis or direct trauma to the affected finger. |
| Do I need to seek medical treatment for my Boutonniere deformity? | The nature of the injury that leads to the deformity means that medical intervention is very important for the proper care of the condition. |
| What types of medications can I rely on to either treat or prevent a Boutonniere deformity? | There are no specific medications indicated in the treatment of Boutonniere deformity. If the condition is the result of rheumatoid arthritis, then anti-inflammatory medications may serve to alleviate the underlying condition and the deformity. |
| Can Boutonniere deformity be permanent? | If left untreated ofr more than three weeks after the initial presentation, there is a strong likelihood that the condition can and will become permanent. |
| Is a Boutonniere deformity the same thing as a mallet finger? | No, the conditions are related and both involve the tendons of the fingers, but they are two distinct conditions. |
| How will Dr. Knight help me with my Boutonniere deformity? | Immobilization in a splint is the most effective and usual treatment, as well as treatment of underlying conditions, followed by therapy. Surgery in more serious cases follows the same trajectory. |
Frequently Asked Questions:
What exactly is Boutonniere Finger and why is it called that?
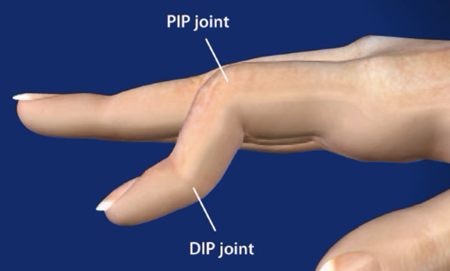
The PIP joint, or Proximal interphalangeal joint, is the middle knuckle of the finger, and a boutonniere deformity occurs when extensor tendon that runs along the top of the finger develops a hole in it, and the PIP joint then pushes through that hole, creating the distinctive deformity of the affected finger that typifies the condition. The condition got its name, because the hole in the tendon through which the PIP joint protrudes resembles a buttonhole, for which the word in French is “boutonnière.” Boutonniere is an anglicized version of this original French word.
Can I cure my Boutonniere Finger without seeing a doctor?
In short, absolutely not. While it is it true that there are some tendon-related conditions that can be treated with rest and icing or wrapping at home, the boutonniere deformity requires medical care and intervention in order to heal correctly. At the earliest stages, before the PIP joint fully protrudes through the buttonhole in the tendon, it may be possible to reverse some of the damage with rest and splinting, but even that would require the oversight of a medical professional in order to affect the best possible treatment. And it is most likely that by the time you notice the deformity beginning to take shape, it is too late for anything other than medical intervention, if not full on surgical intervention.
Is there any medicine for Boutonniere Finger?
Unfortunately, as with many tendon-related conditions that Dr. Knight treats every day, there is no medication that will clear up Boutonniere Finger. If the condition is the result of underlying rheumatoid arthritis, then anti-inflammatory medications may be indicated to treat the underlying cause, but they will have no effect on the torn tendon that is the signature of this condition. Certainly, pain medication can help relieve the discomfort associated with Boutonniere Finger, but it is not a solution, and won’t do anything to actually reverse the damage to your tendon.
Is a Boutonniere Finger the same thing as a Mallet Finger?
No. While a Boutonniere Finger is the result of a hole developing in the extensor tendon over the PIP joint, a mallet finger is when the same tendon is cut or torn over the DIP, or distal interphalangeal joint, which is the last knuckle of the finger. The two conditions present very differently, in regards to the shape of the finger, so a professional can tell them apart from one another easily, but to a layman the initial deformities may resemble one another.
Videos
Animated Videos
(817) 382-6789
Disclaimer
HandAndWristInstitute.com does not offer medical advice. The information presented here is offered for informational purposes only. Read Disclaimer